difficile is also stimulating efforts to address this issue. The increasing threat posed by infections such as C. In-depth analysis of the project has identified other important components of the program, such as rigorous data measurement and feedback and reframing of CLABSI as a social problem in a clinical environment. The combination of improvement in organizational culture and use of the checklist has powered the reductions in CLABSI that have been achieved. Conceptually similar approaches have also been successful in reducing rates of SSIs, and AHRQ is currently funding a large nationwide effort to promote the use of CUSP to reduce rates of CAUTI. The implementation of CUSP to prevent CLABSI has resulted in dramatic nationwide reductions in these serious infections, thanks in part to AHRQ-funded research and dissemination programs that fostered the use of CUSP in intensive care units across the country. CUSP combines improvement in safety culture, teamwork, and communications, together with a checklist that incorporates a manageable set of evidence-based measures to prevent a particular HAI. For example, the development and implementation of the AHRQ-supported Comprehensive Unit-based Safety Program (CUSP) has brought about significant advances in HAI prevention. Organizations that successfully overcome this obstacle represent some of the major successes of the patient safety movement. The challenge has been making it easy for clinicians and health care executives to establish and adopt the recommended methods as standard practice in health care delivery organizations. The CDC has evidence-based guidelines that detail methods to prevent specific HAIs in the inpatient and outpatient setting. What's more, strong evidence links higher hand hygiene rates to lower overall HAI rates. Strategies to improve hand hygiene that rely on traditional educational approaches as well as enhanced monitoring of hand hygiene, feedback on hand hygiene practice in a facility, and sociocultural approaches have resulted in improved hand hygiene at many hospitals and other health care facilities. Although the effectiveness of simple hand washing in preventing infection transmission has been known for decades, until recently hand hygiene rates among all clinicians were low. Prevention of HAIsĪ cornerstone of HAI prevention is appropriate hand hygiene. difficile and antibiotic-resistant bacteria such as methicillin-resistant Staphylococcus aureus (MRSA) is therefore an increasing focus of attention. difficile is now responsible for more than 12% of all HAIs. Infections caused by the bacterium Clostridium difficile have rapidly become more common in hospitals, and C. The CDC's 2011 data indicate that infections associated with specific indwelling devices (CLABSI, CAUTI, and VAP) and SSIs account for approximately half of all HAIs. 
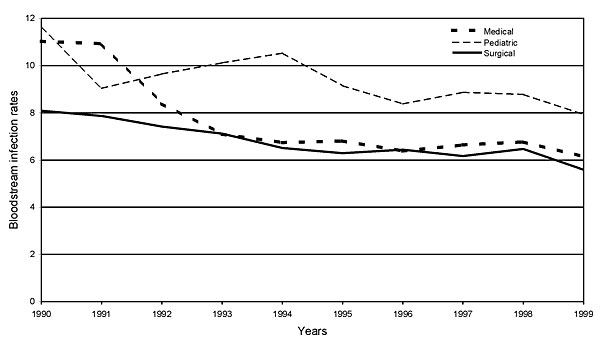
Surgical site infections (SSIs) and infections associated with indwelling devices-ventilator-associated pneumonia (VAP), central line–associated bloodstream infections (CLABSIs), and catheter-associated urinary tract infections (CAUTIs)-have historically account for a large proportion of HAIs, but recent data indicates that the epidemiology of HAIs is evolving. Fortunately, considerable progress has been made in preventing specific HAIs through federally sponsored programs from the Agency for Healthcare Research and Quality (AHRQ), CDC, and the Centers for Medicare and Medicaid Services (CMS). As a result, hospitals and clinicians are prioritizing efforts to reduce the burden of these infections. However, it is now understood that relatively straightforward approaches can prevent many common HAIs. Such infections were long accepted by clinicians as an inevitable hazard of hospitalization. HAIs are estimated to cost billions of dollars annually. These infections can lead to significant morbidity and mortality, with tens of thousands of lives lost each year. More than one million HAIs occur across the United States health care system every year. According to a study by the Centers for Disease Control and Prevention (CDC), at any given time, approximately 1 of every 31 hospitalized patients in the United States has an HAI, meaning that approximately 633,300 patients contract one of these infections annually. Health care–associated infections (HAIs) are among the most common complications of hospital care. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
